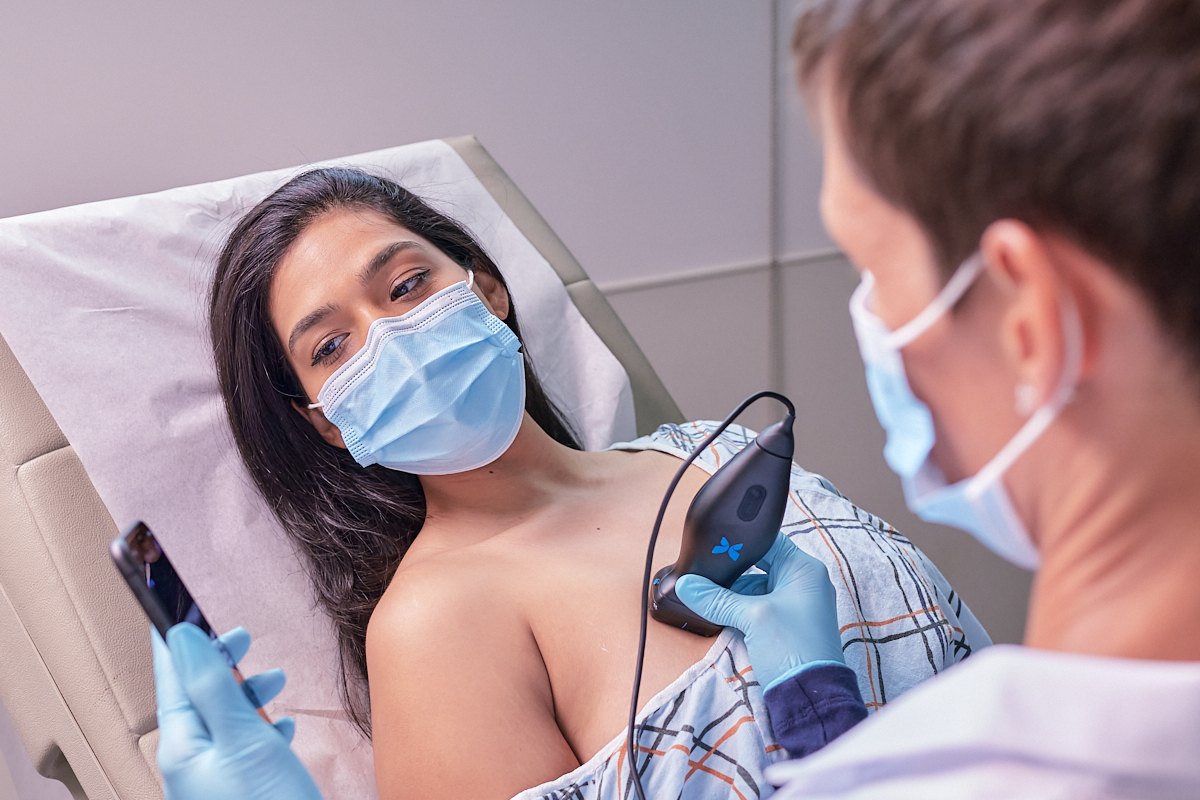
As the health care industry embraces innovative, value-based reimbursement models, there is a growing need to demonstrate value and improved outcomes in care delivery. Recently, Dr. Davinder Ramsingh, vice president of clinical research and development at Butterfly Network, spoke with critical care intensivist Dr. Jared Staab to discuss how innovation at Butterfly is helping drive much needed adoption of point-of-care ultrasound, or POCUS, and how the technology can help payers and providers meet those goals.


Can you tell us a little about POCUS? Specifically, why physicians should embrace it and what health systems should know about it?
POCUS is the application of ultrasound at the bedside, usually performed by the patient’s direct care team. Compared with the typical physical exam that relies on clinical judgment and stethoscopes, and is paired with referrals out for labs, POCUS has shown itself to be faster and more accurate in driving clinical decisions, so it’s an invaluable tool for providers to learn and perform. Misdiagnoses and inefficiency cause direct and indirect physical and financial harm to an already strained health care system, and by leveraging new techniques and advanced technology like POCUS, we can optimize care.
POCUS helps reduce the need for other, more costly and time-consuming, diagnostic tools and labs. These benefits are not only good for the patient; they are good for the entire industry by giving back time and money to patients, providers and hospitals. As we move to health care reimbursement models linked to quality metrics, POCUS will be an important component.
What are some of the most common applications for POCUS that demonstrate its value?
POCUS can be used to enhance the physical exam from head to toe – especially with a device like Butterfly’s that was the first to enable whole-body scanning on one probe. From evaluating intracranial pressure via the optic nerve to looking for deep vein thrombosis in the calves of patients’ legs, POCUS enables fast, accurate diagnosis.
I have taught POCUS for several years in many different locations to very diverse audiences. Interestingly, I’ve seen cardiac ultrasound to be very exciting for many learners, but this enthusiasm is not always as high at the lung ultrasound station… the irony is that lung is one of the easiest applications to learn, and the most relevant to use across specialties.
Mastering lung ultrasound requires committing relatively few variables to memory. It is a tool that offers ease of imaging as well as interpretation, and it can provide superior clinical information compared with the current standard of care for lung evaluation, chest X-ray.
A key benefit compared to X-ray: Lung ultrasound does not require the patient to travel or make unnecessary trips throughout the hospital. We should not forget the lessons of limited diagnostic capability in quarantined environments from the not-so-distant pandemic era. The artifacts encountered in lung ultrasound assist significantly in speeding differential diagnosis without patient travel or ionizing radiation.
As a provider who has adopted lung POCUS as the gold standard for lung assessment, what are the benefits you’ve seen?
Without question, lung ultrasonography provides superior and useful information compared with X-ray. It answers questions related to volume status, fluid tolerance, apnea, pneumothorax associated with trauma and/or central line placement. POCUS is powerful. Within seconds of applying a probe to the chest, the lungs are located, and the practitioner can rule in or out many life-threatening causes of hypoxia and hypotension.
During the most critical times in health care, when every second counts, we are often in dynamic, loud and chaotic environments. These tense, time-sensitive settings are unforgiving when trying to listen for classical auscultation sounds, and it is also not ideal for acute care to pause for a chest X-ray. This is not to say that chest X-rays and stethoscopes have no purpose, but we should no longer rely on those tools in situations that would be better served by a faster and superior tool.
What are some of the barriers to adopting this technology?
I’m disappointed by the slow embrace of POCUS, given vast literature on the low yield and high cost of daily chest X-rays. As with any newer modality that must be adopted by the masses, skill and confidence can be a barrier. We have a generation of practitioners in the field with minimal ultrasound experience. Fortunately, with the increasing incorporation of POCUS instruction into UGME and GME training, the knowledge and skill gap continue to close.
At the same time, the cost and footprint of bedside ultrasound continues to improve – Butterfly’s device is a great demonstration of this. With a single probe, it enables full-body scanning for less than $3,000 whereas traditional handhelds require multiple probes at higher costs, and carts have significantly higher costs than handhelds. POCUS solutions, especially smaller handheld platforms like Butterfly’s, represent much-needed disruptive innovation in health care, helping address not only the problem of access to technology, but also tackling challenges with proficiency management, security, cloud storage and workflow optimizations.
Butterfly is focused on helping overcome these barriers by boosting ultrasound competency and confidence with AI tools and educational support. What is your experience with these?
AI and machine learning are increasing the uptake and value of POCUS in many ways. Such tools – for example the AI-enabled Auto B-line Counter that Butterfly recently released for lung assessment – add speed, consistency and standardization to scanning, diagnosis and treatment monitoring.
Further, POCUS, like any skill, needs to be nurtured and maintained; if you don’t use it, you lose it. So, resources, like Butterfly’s educational modules and hand-on training programs are important additions to the POCUS landscape, helping scale training so more providers confidently embrace ultrasound.
We are surrounded by rising health care costs and increasing patient complexity, while time spent in training has remained static. In this environment, it is critical to embrace POCUS, and I applaud Butterfly for working diligently to integrate novel machine learning and AI diagnostic and educational techniques. Efficiency in education and clinical practice will save lives.
Dr. Jared Staab practices as an intensivist and anesthesiologist. He also assumes the pivotal roles of residency program director, associate program director for the critical care fellowship program director and Director of Innovation at the University of Kansas Medical Center Department of Anesthesiology. Dr. Staab has been instrumental in pioneering the ultrasound training programs for both the critical care fellowship and anesthesiology residents, bringing transformative changes to their health system.
Dr. Davinder Ramsingh is the vice president of Clinical Research and Development at Butterfly Network, a professor of anesthesiology at Loma Linda Medical Center, and is an avid author and lecturer of medical ultrasound research and education.
℞ only. Butterfly iQ/iQ+™ is a portable ultrasound system designed for external ultrasound imaging. Read the User Manual for the warnings, precautions and/or contraindications. Learn more about Butterfly Network here.