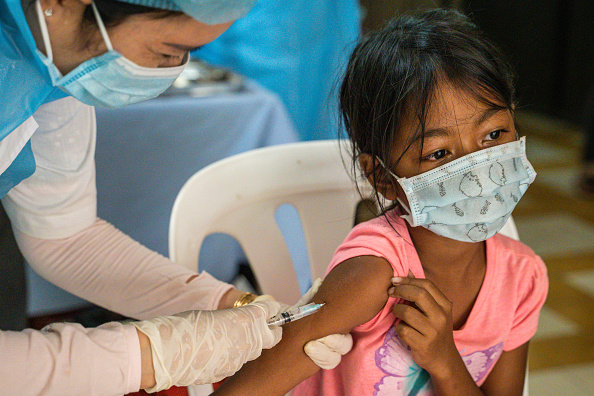
As pediatric practices adapted in the early weeks of the pandemic and fears of coronavirus exposure kept parents and children home, routine health care was delayed across the country. More than two years later, missed routine childhood vaccination may be one of the most concerning consequences of those delays.
While practices generally resumed routine care as quickly as public health guidelines would allow, not all children immediately returned. More than 40% of parents surveyed in March 2021 said their youngest child had missed a routine health care visit due to the pandemic. Such delays “could have significant long-term impact on the health of children, their families and communities,” epidemiologist Chloe Teasdale and colleagues wrote in the paper.
Well-child visits are critical to providing information about and administration of vaccines. The vaccines recommended by the US Advisory Committee on Immunization Practices for children under age 2 protect against more than a dozen infectious diseases. In addition, vaccines recommended for older children also guard against the long-term threat posed by diseases like cervical cancer. However, vaccine hesitancy meant protection against some diseases was waning even before the pandemic, leaving children and vulnerable adults unprotected as preventable diseases like whooping cough and measles became more common.
Reports that pediatric vaccination has suffered through the pandemic suggest public health could be at risk, and experts say pediatricians must prioritize bringing children up to date. Best practices from pediatricians that have maintained or improved vaccination coverage though the pandemic may help.
How did the pandemic affect routine childhood immunization?
Vaccination at eight US health systems dropped substantially in the first several months of the pandemic, according to one study. Vaccination remained below normal levels across most age groups into fall 2020. Even among groups where vaccination rebounded, fewer children were up to date in September 2020, compared with September 2019. Black children were least likely to be up to date on vaccines, another example of the pandemic’s heavy toll on families of color.
The issue appears to have persisted into the pandemic’s later months. For example, 30.9% of Minnesota 2-year-olds were not up to date on routine shots in 2021, compared with 20.3% prior to the pandemic. The March 2021 survey of parents found that one-third reported their child had missed a vaccine. And an Avalere analysis found that vaccination briefly increased in March 2021 but otherwise remained consistently below 2019 levels. Routine vaccination has also waned around the world, sparking concern from the World Health Organization and the United Nations Children’s Fund.
However, the trend has not been uniform. Nemours Children’s Health, for example, saw year-over-year year-end vaccine uptake rates increase in 2020 and again in 2021. Rates for 2022 appear to largely be up as well, although flu vaccination uptake has dipped.
That success may stem largely from the protocols Nemours practices implemented early in the pandemic. Teams developed cohort care models that segmented well children from those who were sick, and they stood up tents for the in-person portion of well-child care, including administration of vaccines.
With children attending school remotely and families avoiding public gatherings, the typical flu-season schedule eased. In turn, Nemours practices were able to devote more time to well-child care, and care coordinators were charged with making contact with families whose children were behind on routine care. That meant children who had missed recommended vaccines were identified, and Nemours clinicians took steps to bring them up to date.
The American Academy of Pediatrics advises pediatricians to identify children who are behind on routine vaccines and bring them up to date as soon as possible. As other pediatric practices work to catch children up, lessons from the Nemours experience may prove helpful.
Regaining ground on routine vaccination
Examining the reasons behind waning vaccination rates may provide a starting place for outreach to bring children up to date.
Confusion and misinformation seem to be important factors. While practices quickly figured out how to provide care safely even as COVID-19 spread, confusion persisted among parents about whether and when to bring children into the doctor’s office, experts say. Scheduling and child care challenges also played a role as parents’ lives were upended by the crisis.
However, even when children came in for care, they were not always vaccinated. Again misinformation – and the mistrust it fosters – may be partly to blame.
COVID-19 vaccine hesitancy is widely believed to have hindered the fight against the pandemic, but it also seems to have spilled over into willingness to have children immunized against other infectious diseases, says Dr. Jonathan Miller, medical director of value-based care and chief of primary care at Nemours Children’s Health Delaware Valley. Now, as masks come off, Miller is concerned that vaccine-preventable diseases like measles that were muffled by public health measures could resurface.
Miller says pediatricians themselves have the power to help turn the tide. “I think providers who are passionate about vaccines and who provide a strong recommendation for vaccines get a much better response and much better uptake of vaccines,” he said. “If you give a strong recommendation; if you are persistent in your recommendation over time, don’t just take no (for an answer), but if you come back and revisit it … a lot of people will come around.”
The AAP says well-child visits should occur in person when possible, but even telehealth visits are a chance to remind patients and parents about vaccines. And physician Sandra Fryhofer suggests physicians bring up vaccination status during telehealth calls and administer vaccines even when in-office care is scheduled for another purpose.
That’s the approach taken by Nemours clinicians, who bring up vaccines any time they interact with a patient for any reason. Miller said an EMR prompt added as part of Nemours’ systemwide quality improvement work also keeps vaccines top of mind.
Here are some other recommendations Miller shared:
- Collect – and act on – data: Miller says leveraging EMR data to examine vaccination status across a patient population is key to improving immunization rates. Once practices understand the demographics, they may be able to design interventions that are more effective, including interventions to address social disparities.
- Assign a point person for outreach: Not all practices will be able to assign embedded care coordinators to reach out to parents whose children have fallen behind on routine care. That’s OK, Miller said. Just designate someone in the practice to own this work and set aside some time to focus on it.
- Vaccinate at scale: Miller said analysis of vaccination status may identify clear cohorts of children who are behind on immunizations. He suggests looking for strategies to make progress quickly, just as many practices did early in the COVID-19 vaccine rollout. COVID-19 vaccination clinics allowed rapid immunization of many children, and the idea could be adapted for routine vaccines as well.
- Think outside the care-site box: The COVID-19 pandemic has demonstrated how rapidly vaccination can occur when shots are administered outside the walls of a primary care practice. At Nemours, flu shots are given in specialty clinics, emergency departments and inpatient floors, for example. In the community, Miller says schools can be a great place to reach children with routine vaccines. “We know we only see a certain percentage of our patients each year for well visits, so you’ve got to get to them in other places, too,” he said.
Practices working to boost vaccination rates can also turn to resources from the AAP, including communication strategies for combating vaccine hesitancy, best practices for patient reminders and recall systems, advice for handling resistance to vaccination and other tools. Strategies for discussing COVID-19 vaccines with parents may translate to other vaccine conversations. Regardless of the specific tactic, Fryhofer urged colleagues in an American Medical Association video update to “come up with a plan, be creative, be efficient.”
If you liked this article, sign up for Pediatrics Today SmartBrief. It’s among SmartBrief’s more than 250 free industry-focused email newsletters.
Melissa Turner is a health care editor at SmartBrief. Connect with her on LinkedIn.