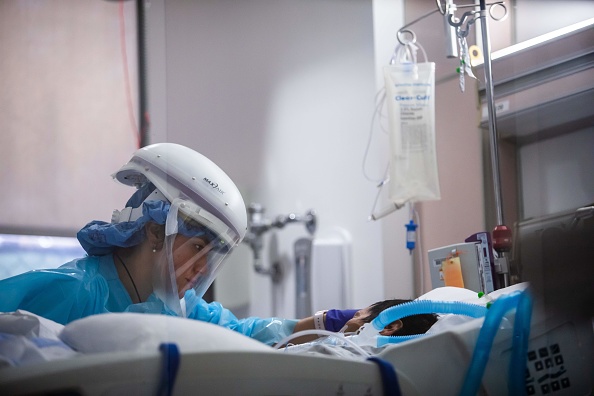
Critical Care SmartBrief readers this past week weighed in on the following survey question:
What’s one new, successful protocol or workflow your facility has implemented amid the COVID-19 pandemic?
Their insights and answers:
- As best we can. It takes a powerful, engaged leadership group to start and sustain the effort.
- Ignore.
- Decreasing the workload; providing supplies and security measures.
- We have not done anything.
- No.
- Our hospital has a counseling team available for burnout and acute stress from COVID, free of charge and confidential. I utilized it myself last spring.
- They really haven’t addressed these issues. I was the only doctor caring for 30-plus critically ill patients with 1-2 APP’s in January. I started my day at 7 a.m. and ended my day at 1 a.m. with no extra money for staying past 7 p.m. The people in charge don’t understand how difficult it is to care for more than 12-14 critically ill patients in a 12-hour shift, but they want that $460 per hour reimbursement from Medicare ($230 for each 30 minutes of critical care) for the intensivist’s work while paying only $175-200 per hour to the doctor who is working like a dog. And then they wonder why there is a 51% burnout rate in Intensivist physicians.
- This has not been addressed.
- Offered a number to seek free counseling.
- No.
- Nothing. Just a “tranquility” room.
See this week’s brief for the next survey question and be sure to submit a response.
____________________________________
Kathryn Doherty has been a health editor with SmartBrief for 15 years. She has covered many facets of the health care industry during that time and currently focuses on physicians, health care providers, nutrition and wellness.
Sign up for Critical Care SmartBrief for more critical care news, research and commentary. And for more health care content delivered straight to your inbox, check out all of SmartBrief’s health care newsletters, covering health IT, news for insurers, news for health care providers and more.