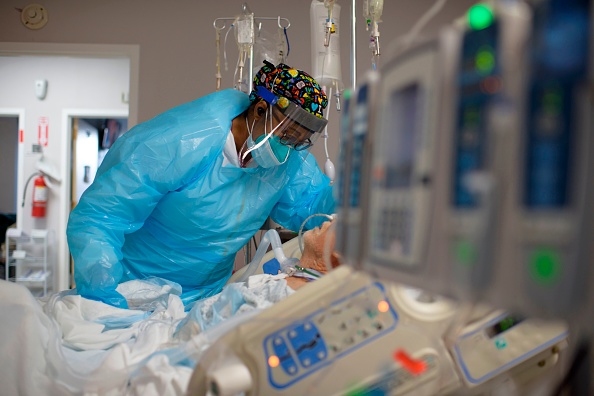
Providence Regional Medical Center in Everett, Wash., identified the United States’ first known COVID-19 patient on January 20, 2020, marking the onset of a health care crisis whose proportions would have been difficult to imagine at the time. Soon afterward, the health system also took on a pioneering role in treating COVID-19 patients with the antiviral drug remdesivir.
As of April 2022, the US has counted 81 million cases of coronavirus infection and almost 1 million deaths – nearly a sixth of the world’s total lives lost to date – and the pandemic has done no less than permanently alter the way health care organizations operate and practice medicine.
In a conversation with SmartBrief, Darren Redick, chief executive of the Providence Swedish North Puget Sound health system, offered some constructive hindsight on challenges the crisis has presented and solutions his organization found to address them.
SB: Looking back on the last two years, what has Providence learned about handling the high-stress and high-volume patient care demands of a pandemic? What processes and precautions did you already have in place before the COVID-19 crisis?

DR: As the hospital that admitted the first known COVID-19 patient in the United States, Providence Everett has been on the frontlines of the pandemic from the very beginning. We were uniquely prepared, however, and our Biocontainment, Evaluation, and Specialty Treatment (BEST) team had just run through a full drill two weeks prior to the first patient arriving, in which they practiced receiving and caring for an infectious disease patient. We have a special unit we can set up for infectious disease patients, and that unit was used for the first COVID patient. For years, we have done regular drills for that unit – going back to when we were preparing for the possibility of an Ebola patient. Our drills include our community partners, such as the Health District, EMS, the Northwest Healthcare Response Network, and more. One reason the process for the initial patient went well is the drill we had a couple of weeks prior included our community partners.
We also have a medical tower that was designed with a pandemic in mind, so an entire floor has reverse air flow capabilities. These “pandemic HVAC systems” are available for 64 beds across two units. In addition, as part of the Providence health system, we had a relatively good supply of PPE available. These factors have been extremely helpful throughout the pandemic to help limit exposures in the hospital. The high-stress and high-volume demands of the pandemic have been extremely difficult, but our caregivers have endured with compassion and strength, and I am so proud of them and humbled to work with them. Our Providence mission calls for us to be steadfast in serving all, and our caregivers have indeed provided excellent care throughout the pandemic.
Also, for years we have had in place a Service Operations and Transfer Center to manage operations, and that has proven invaluable throughout the pandemic.
SB: When the next pandemic arrives, how will your staff and facilities be better prepared for it? Have you added equipment, permanent training programs, more treatment space, technology, other tools that can help?
DR: Health care has been fundamentally altered by the pandemic in many ways. For example, we quickly pivoted to provide many telehealth and virtual care options for our patients during the pandemic, and many of those programs will continue. This is a great option for many patients and also allows resources to be deployed to more critical patients. Specifically, at Providence Everett, we have developed many new training programs and protocols around infection prevention, care and treatment of infectious disease patients, and more. We also have the ability to quickly flex and adjust our operations based on the situation. All of these experiences, and many more, will be important as we face future COVID-19 surges, another pandemic, or other challenges.
From a building system standpoint, I think we have also been well prepared. We understand that health care is a larger, connected system and that impacts to any portion of the system (primary care, specialty care, ambulatory care, post-acute services, long term care services) all affect one another. As a community of health care services and organizations, it is clear we need to plan and work together to best manage the effects of pandemics and other critical community health issues.
SB: What is it like handling the psychological uncertainty and stress of a pandemic – especially when you know more infectious diseases will appear, but you don’t know how much differently they will present, or how severe they will be?
DR: The uncertainty and stress for all frontline health care workers has been intense, and Providence has implemented a multitude of programs and resources to help with mental health concerns, child care challenges, work-life balance, and much more. As a specific example, we have trained and deployed Critical Incident Stress Management teams to help caregivers after they have been through a difficult situation. These teams allow caregivers to debrief after an incident, share how they’re feeling, be connected to resources, and more. Our caregivers are here because they are passionate about caring for others. Health care is a calling, and that has never been more apparent than during the last two years.
SB: Were there any pandemic protocols or technologies that you thought would be effective in managing patient care, but that turned out to be less helpful? What did you learn from those situations?
DR: Throughout the pandemic we have followed guidance from the CDC and the Department of Health, which is based on evidence-based best practices. The entire world has seen science play out in real time throughout the pandemic, and we’ve all learned that the process is not always linear. However, by following proven treatments and established protocols, we have provided excellent care to our patients.
SB: What kinds of organizations have you partnered with to educate and prepare staff and the hospital for future outbreaks?
DR: Beginning with the very first COVID patient – and even before that, during drills – we worked closely with our local health department, EMS, fire department, and more. Throughout the pandemic, we’ve partnered with other hospitals in the state to level patient load so that no single hospital got overwhelmed during a surge. This helped keep Washington state from declaring crisis standards of care. This coordination of care among hospitals and health organizations throughout our state is extremely important and has positioned us well for future challenges.
SB: Have other hospitals approached you to advise them on establishing better pandemic protocols? If so, how do you handle those requests?
DR: Since we successfully treated the first COVID-19 patient in the US, we’ve been getting calls from other hospitals around the country for two years. Health care is all about sharing information and best practices to help advance patient outcomes. For example, in March 2020, our team published a case report of the first patient in the New England Journal of Medicine to help share our experience and how the patient was successfully treated with remdesivir. Throughout the pandemic, we have also worked closely with the Washington State Hospital Association to share information, and WSHA has done a tremendous job helping hospitals coordinate and respond.
SB: What have been the most rewarding and encouraging outcomes from your preparedness efforts? Can you share any data or study results on efficiencies, cost savings, patient health impact?
DR: The most rewarding and encouraging part is the stories of the patients who recover. For example, USA Today featured this story of a Providence Everett patient who spent 25 days on a ventilator, but made a full recovery and was reunited with her family. Knowing that the drills and the training, the protocols and procedures, the foresight to have a floor with reverse air flow, and most of all, the dedication, care, bravery and expertise of our caregivers, all played a role in saving so many lives is extremely powerful. Throughout the pandemic, we have also been at the forefront of research and new therapies.
We were the first in the world to administer remdesivir to a COVID-19 patient. We have published numerous studies about care and treatment of COVID-19, and shared a lot of information with the public to help educate them and promote best practices. Examples include this paper on Remdesivir and Mortality Rates in Patients with COVID, as well as this account on the role of technology in COVID-19 care and delivery.
If you liked this article, sign up for SmartBrief for Health Care Leaders. It’s among SmartBrief’s more than 250 free industry-focused email newsletters.